
Medically Reviewed By
Karen Ritter, RN BSN
Registered Nurse
JUMP TO A TOPIC
![]()
Important Facts About Malignant Peritoneal Mesothelioma
- Peritoneal mesothelioma is a cancer of the peritoneum, which is a sheet-like membrane surrounding your abdominal cavity.
- Peritoneal mesothelioma accounts for between 10% and 15% of all mesothelioma cases, making it the second most common form of mesothelioma.
- Peritoneal mesothelioma patients have longer life expectancies than those with other types of mesothelioma.
- The average age for patients with malignant peritoneal mesothelioma is 57, and 56% are male.
What Is Malignant Peritoneal Mesothelioma?
Malignant peritoneal mesothelioma is a cancerous, fast-spreading disease that can spread throughout the abdomen.
Peritoneal mesothelioma causes abnormal mesothelial cells to divide uncontrollably. These fast-growing cells form clumps of cells called tumors, which affect the surface and organs inside the abdominal cavity.
Tumors can be malignant (cancerous), such as sarcomatoid and epithelioid, or benign (not cancerous).
Causes of Peritoneal Mesothelioma
Exposure to asbestos is a risk factor for malignant mesothelioma. This type of cancer is associated with inhaling (breathing in) or ingesting (swallowing) asbestos.
Dr. Shanel Bhagwandin, a peritoneal mesothelioma specialist, explained how fibers reach the abdomen.
“As far as how (asbestos fibers) might reach the abdomen and result in cancer, it could be anything from swallowing the fibers, and they travel through the digestive tract and reach the peritoneum.” — Dr. Shanel Bhagwandin
The average age for peritoneal mesothelioma patients is 57, and approximately 56% are male. Peritoneal mesothelioma affects females more than pleural mesothelioma does.
How Does Peritoneal Mesothelioma Develop?
Peritoneal mesothelioma develops through a multi-step process. It starts with a history of asbestos exposure. Asbestos fibers enter the body, causing genetic changes to cells:
1
Asbestos fibers are inhaled or ingested.
2
The sharp fibers lodge into tissue along either side of your peritoneum.
3
Genetic damage prevents cells from regulating their replication, which causes tumors to form.
Peritoneal mesothelioma typically remains in the abdomen, but the disease can spread to the lungs.
Symptoms of Peritoneal Mesothelioma
Symptoms of peritoneal mesothelioma may not occur right away and are often vague. The cancer is often undetectable until it has developed large tumors or the cancer has spread throughout the peritoneal cavity. One common symptom is the buildup of fluid in the abdomen, called ascites.
Other symptoms of peritoneal mesothelioma may include:
- Abdominal pain
- Constipation or bowel obstruction
- Nausea
- Vomiting
- Unexplained weight loss
- Loss of appetite
- Fever
- Abdominal swelling
- Fatigue
- Shortness of breath
Peritoneal Mesothelioma Diagnosis
Diagnosing peritoneal mesothelioma can be difficult since symptoms are often vague and similar to other health conditions. Mesothelioma of the peritoneum can be confused with abdominal distension (gas) and irritable bowel syndrome. Unfortunately, because of the nonspecific symptoms and the rarity of the disease, mesothelioma is usually diagnosed late, and the disease burden is extensive.
To receive an accurate diagnosis of peritoneal mesothelioma doctors rely on abdominal X-rays, CT Scans (computed tomography), MRIs and PET scans.
Peritoneal mesothelioma is diagnosed with a tissue biopsy. Doctors may choose to use a laparoscopy to perform the biopsy. Surgeons make small incisions in the patient’s abdomen and then use a camera to explore the abdominal cavity. There are small instruments that can be inserted through the small incisions to help extract tissue samples to test for peritoneal mesothelioma.
Peritoneal mesothelioma is diagnosed with a tissue biopsy. A CT-guided core needle biopsy is a less invasive way to obtain tissue and confirm a peritoneal mesothelioma diagnosis. If a core needle biopsy is not possible, doctors may choose to use a diagnostic laparoscopy to obtain biopsy tissue samples.
Surgeons make small incisions in the patient’s abdomen and then use a camera to explore the abdominal cavity. There are small instruments that can be inserted through the laparoscope to help extract tissue to test for the presence of peritoneal mesothelioma.
Peritoneal Cancer Index
Mesothelioma staging differs based on the type of the disease. For pleural mesothelioma, doctors assign a number between 1 and 4. Stage 1 is the least severe and stage 4 is the most severe.
Specialists use a separate staging system for peritoneal mesothelioma: the peritoneal cancer index, which scores the disease spread within the abdominal cavity.
13 Sections of the Abdominal Cavity


There are 13 sections of the cavity, and each one receives a score between 0 and 3. The score depends on the size and number of tumors in that space. A score of 0 means no cancer exists in that section, and a score of 3 means there is widespread disease in that area. The scores are added up to a total, which is assigned to a stage:
PCI Score
Stage
1 - 10
11 - 20
21 - 30
31 and higher
Stage 1
Stage 2
Stage 3
Stage 4
Sample PCI Score Chart

PCI Score
Stage
1 - 10
11 - 20
21 - 30
31 and higher
Stage 1
Stage 2
Stage 3
Stage 4
PCI Score: 8
Stage 1
The score and equivalent stage help specialists determine the treatment. Curative treatment options, like cytoreduction surgery, are typically for patients with limited disease or a low PCI score that shows the disease is not in unfavorable locations (small bowel, the vessels or the liver’s bile duct).
Patients with more advanced disease receive palliative (symptom-relieving) treatments. An example of palliative treatment is paracentesis, which drains fluid from the abdomen.
Treatment of Peritoneal Mesothelioma
The standard treatment options for peritoneal mesothelioma include surgery and chemotherapy. There are additional treatments available to patients through clinical trials. Finding cancer treatment from a specialist is a crucial step after receiving a diagnosis of peritoneal mesothelioma.
Cytoreduction surgery is the primary treatment option for peritoneal mesothelioma. This involves debulking, or removing all visible tumors and any diseased tissue. Surgeons also often remove the patient’s peritoneum, where peritoneal mesothelioma forms.
Chemotherapy is a common treatment for peritoneal mesothelioma. There are two methods: intravenous or intraperitoneal.
Surgery for Peritoneal Mesothelioma
The primary surgery option for peritoneal mesothelioma is cytoreductive surgery with hyperthermic intraperitoneal chemotherapy.
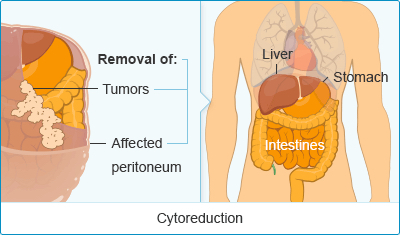
Cytoreduction Surgery
Cytoreduction surgery is the primary treatment option for peritoneal mesothelioma, which involves debulking (removing) all visible tumors and diseased tissue in the abdominal cavity.
The goal of cytoreduction is to remove all visible tumors and diseased tissue. Surgeons remove the patient’s peritoneum, where peritoneal mesothelioma forms, and may need to remove part of the intestines or other abdominal organs. This surgery is commonly combined with HIPEC to destroy any microscopic cancer cells remaining after the surgical removal of tumors.
Cytoreduction is an extensive procedure, often taking surgeons up to 12 hours to complete.
Inpatient recovery can take anywhere from 1-2 weeks. Once patients return home, they may need one to two months for full recovery. Patients with more disease or higher PCI scores will often require a longer procedure with more debulking which is often associated with higher complication rates.
Post-surgery effects such as nausea, vomiting, constipation and fatigue can last for months after surgery. With the advances in anesthesia and post-operative care, mortality is less than 1%.
Heated Intraperitoneal Chemotherapy (HIPEC)
HIPEC is hyperthermic intraperitoneal chemotherapy used to treat peritoneal cancers or cancer of the abdomen. The HIPEC procedure introduces both heat and chemotherapy which work together to kill tumor cells.
The chemotherapy solution is directly pumped into the abdominal cavity, allowing for the use of high doses of chemotherapy. This chemotherapy technique helps to kill cancer cells remaining after cytoreduction without the side effects that are typically associated with traditional chemotherapy.
HIPEC Treatment in Action
HIPEC treatment may vary depending on the facility. The MD Anderson Cancer Center website says surgeons heat cisplatin, the intraperitoneal chemotherapy for peritoneal mesothelioma, to 103 degrees Fahrenheit. They then rock the patient back and forth to ensure the drug washes the entire abdomen.
According to the cancer center, around 90% of the liquid cisplatin stays within the abdominal cavity. This reduces the negative effects on other body areas.
A study conducted by Dr. Sugarbaker, the innovator of this procedure, proved cytoreduction and HIPEC are successful in treating malignant peritoneal mesothelioma. Of 405 patients in the study, 60% had a three-year survival rate, and 47% had a five-year survival rate. The overall median survival was 53 months.
Chemotherapy for Peritoneal Mesothelioma
Chemotherapy for peritoneal mesothelioma often includes a combination of pemetrexed and cisplatin. These two chemotherapy drugs are approved by the U.S. Food and Drug Administration for peritoneal mesothelioma treatment.
A combination of both chemotherapy drugs is usually best. In one study, 41% of patients who were given the combination experienced improved survival. Only 17% showed satisfactory results after receiving just cisplatin.
On average, the combination of pemetrexed and cisplatin helped patients live 12.1 months longer compared to no chemotherapy.
Studies are also testing other chemotherapy drugs — such as vinorelbine and gemcitabine — with cisplatin.
Peritoneal Mesothelioma Survival Rates
Although there isn’t a cure for mesothelioma, many patients have a hopeful peritoneal mesothelioma prognosis.
There are cases of long-term survivors in remission for more than 15 years. Kendra Ferreira, for instance, was diagnosed in 2001 and has far outlived her mesothelioma prognosis
The most successful outcomes involve the detection of mesothelioma in earlier stages. Early diagnosis means there is limited presence of cancer, so treatment begins immediately. According to a study, the five-year survival for patients diagnosed with stage 1 (PCI score of 1-10) was 87%.
In an analysis of 2,000 peritoneal mesothelioma patients registered in the National Cancer Database, radical surgery plus systemic chemotherapy led to a median survival of 41 months. Patients who didn’t receive surgery often survived for less than one year.
Patient outcomes are directly related to the doctor’s expertise. Mesothelioma is a rare and aggressive cancer and requires years of experience to accurately diagnose and treat.
Patients are best treated at specialty cancer centers that work in a multidisciplinary setting with input from medical oncologists, surgical oncology, radiation oncologists, pathologists, radiologists, genetic counselors and dieticians.
Learn how mesothelioma survivors beat the odds in our free Mesothelioma Survivors Guide. You’ll read the stories of multiple people who have outlasted their mesothelioma prognosis and continue to live enriching lives.
If you would like more information about mesothelioma and your treatment options contact one of our patient advocates. You can email our registered nurse, Karen Ritter, at karen@mesotheliomaguide.com.
Veterans With Peritoneal Mesothelioma
Veterans comprise the largest group of people who have mesothelioma. Approximately one-third of U.S. mesothelioma cases are former military members.
The U.S. Department of Veterans Affairs (VA) offers numerous benefits to veterans who have peritoneal mesothelioma. If the disease formed due to service-related asbestos exposure, then the veteran could receive Disability Compensation.
If you are a veteran with peritoneal mesothelioma — or a survivor of a veteran who passed away due to this cancer — our VA Accredited Claims Agent can help you. Contact us today or request our free Veterans Support Guide.
Frequently Asked Questions About Peritoneal Mesothelioma
How is a patient diagnosed with peritoneal mesothelioma?
Peritoneal mesothelioma symptoms are often nonspecific and can be similar to other health conditions. Peritoneal mesothelioma is a rare cancer so it is important to identify your symptoms and seek a medical evaluation and testing.

What is the prognosis for peritoneal mesothelioma patients?
The average life expectancy for peritoneal mesothelioma is around one year, but early detection and aggressive treatment can lead to survival lengths of five or more years. Women and younger patients tend to live for longer. There is currently no cure for peritoneal mesothelioma.
How does peritoneal mesothelioma form?
Asbestos exposure is the only known link to peritoneal mesothelioma. Loose, sharp fibers pierce into cell linings and irritate tissue, which can cause genetic mutations. When asbestos particles are inhaled or swallowed, they can reach the peritoneum. This thin membrane, which lines the abdominal cavity, is where peritoneal mesothelioma forms.
Who is most likely to get peritoneal mesothelioma?
Males make up a little more than half of the people with peritoneal mesothelioma. The average age of patients is around 52. People who worked with asbestos — or the loved ones of exposed to asbestos — are most at risk of this cancer.
How is peritoneal mesothelioma treated?
Doctors use a combination of surgery and chemotherapy to achieve the best overall survival for people with peritoneal mesothelioma. The method is cytoreduction with hyperthermic intraperitoneal chemotherapy.
Sources & Author
- Malignant peritoneal mesothelioma: Epidemiology, risk factors, clinical presentation, diagnosis, and staging. UpToDate. Retrieved from: https://www.uptodate.com/contents/malignant-peritoneal-mesothelioma-epidemiology-risk-factors-clinical-presentation-diagnosis-and-staging?search=mesothelioma%20statistics&source=search_result&selectedTitle=1~74&usage_type=default&display_rank=1. Accessed: 03/19/19.
- Signs and Symptoms of Mesothelioma. American Cancer Society. Retrieved from: https://www.cancer.org/cancer/malignant-mesothelioma/detection-diagnosis-staging/signs-symptoms.html. Accessed: 04/10/19.
- Mesothelioma: Symptoms and Signs. American Society of Clinical Oncology. Retrieved from: https://www.cancer.net/cancer-types/mesothelioma/symptoms-and-signs. Accessed: 04/10/19.
- Tests for Malignant Mesothelioma. American Cancer Society. Retrieved from: https://www.cancer.org/cancer/malignant-mesothelioma/detection-diagnosis-staging/how-diagnosed.html. Accessed: 04/10/19.
- Determining the Peritoneal Cancer Index. HIPEC.com. Retrieved from: http://www.hipec.com/knowledge-base/determining-the-peritoneal-cancer-index/. Accessed: 04/12/19.
- Cytoreductive surgery with hyperthermic intraperitoneal chemotherapy for peritoneal mesothelioma: patient selection and special considerations. Cancer Management and Research. Retrieved from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6511620/#CIT0023. Accessed: 02/4/20.
- HIPEC Surgery – What to Expect. Tufts Medical Center. Retrieved from: https://www.tuftsmedicalcenter.org/patient-care-services/Departments-and-Services/Cancer-Center/Clinical-Care-Services/Peritoneal-Surface-Malignancy-Program/What-to-Expect-After-HIPEC-Surgery. Accessed: 05/15/19.
- Hyperthermic Intraperitoneal Chemotherapy. MD Anderson Cancer Center. Retrieved from: https://www.mdanderson.org/treatment-options/hyperthermic-intraperitoneal-chemotherapy.html. Accessed: 03/13/18.
- Malignant peritoneal mesothelioma: Treatment. UpToDate. Retrieved from: https://www.uptodate.com/contents/malignant-peritoneal-mesothelioma-treatment?source=bookmarks_widget. Accessed: 03/13/18.
- Life Expectancy in Pleural and Peritoneal Mesothelioma. Lung Cancer International. Retrieved from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5292397/. Accessed: 03/19/19.
- Molecular Pathways and Diagnosis in Malignant Mesothelioma: A Review of the 14th International Conference of the International Mesothelioma Interest Group. Lung Cancer. Retrieved from: https://www.researchgate.net/publication/329200715_Molecular_Pathways_and_Diagnosis_in_Malignant_Mesothelioma. Accessed: 03/19/19.
- Predictors and Outcomes of Surgery in Peritoneal Mesothelioma: An Analysis of 2000 Patients From the National Cancer Database. Annals of Surgical Oncology. Retrieved from: https://pubmed.ncbi.nlm.nih.gov/32006127/. Accessed: 02/04/20.














